Click on "Objectives Ch. 15" tab to take you to the objectives sheet for this chapter.
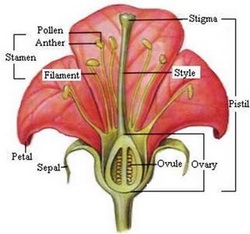
Objective 1 - plant structure
Male Structure - Stamen (made up of anther (containing pollen) and filament)
anther - top part of stamen that contains pollen.
filament - stalk that holds the anther.
pollen - powdery substance that contains male gametophyte (sperm) and can be carried by wind or insects to the plants it fertilizes.
Female Structure - Pistil (made of up stigma, style, and ovary)
Ovary contains ovule (seeds)
stigma - top portion of pistil (often sticky) on which male pollen grains are deposited.
style - slender part of the pistil between stigma and ovary.
ovary - lower part of the pistil, contains ovules and develops into fruit of plant.
Fruit – an enlarged ovary that contains seeds. The fruit is a fleshy part of the plant often used to attract
animals.
ovule - tiny structures in a seed plant found in the ovary that develop into the seed after fertilization.
Male Structure - Stamen (made up of anther (containing pollen) and filament)
anther - top part of stamen that contains pollen.
filament - stalk that holds the anther.
pollen - powdery substance that contains male gametophyte (sperm) and can be carried by wind or insects to the plants it fertilizes.
Female Structure - Pistil (made of up stigma, style, and ovary)
Ovary contains ovule (seeds)
stigma - top portion of pistil (often sticky) on which male pollen grains are deposited.
style - slender part of the pistil between stigma and ovary.
ovary - lower part of the pistil, contains ovules and develops into fruit of plant.
Fruit – an enlarged ovary that contains seeds. The fruit is a fleshy part of the plant often used to attract
animals.
ovule - tiny structures in a seed plant found in the ovary that develop into the seed after fertilization.
Objective #2
Plant Reproduction - p. 174-76 (these notes were given in class)
Sexual Reproduction:
•Pollen grain reaches stigma – pollination
•Pollen grain grows a pollen tube to carry sperm cells down the style to ovules in the ovary.
•Sperm and egg unite –zygote
•As zygote grows (embryo) wall of ovule hardens into seed coat
•Ovary develops into fruit
Note:
•2 sperm cells are needed
– One unites with egg
– Other combines with 2 haploid nuclei to form endosperm
• endosperm is rich in starch and food reserves. “nutrient storage”
**two types of questions on public:
–Structure
–Number of sperm, haploid nuclei, etc.
Plant Reproduction - p. 174-76 (these notes were given in class)
Sexual Reproduction:
•Pollen grain reaches stigma – pollination
•Pollen grain grows a pollen tube to carry sperm cells down the style to ovules in the ovary.
•Sperm and egg unite –zygote
•As zygote grows (embryo) wall of ovule hardens into seed coat
•Ovary develops into fruit
Note:
•2 sperm cells are needed
– One unites with egg
– Other combines with 2 haploid nuclei to form endosperm
• endosperm is rich in starch and food reserves. “nutrient storage”
**two types of questions on public:
–Structure
–Number of sperm, haploid nuclei, etc.
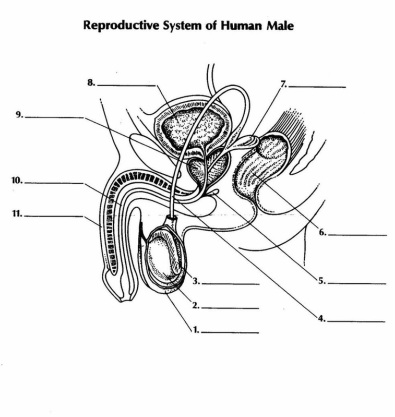
Objective 3 - Originally set for homework. Identify structures based on numbers next to definitions.
2. testes
- outside the body cavity
–produce male gamete (sperm) and reproductive hormones
–develop in the body cavity but descend into the ...
1. scrotum
- external sac which surrounds the testes
–allows the testes to remain ~ 1.5 degrees celcius below body temp for normal sperm production
•seminiferous tubules
- long coiled tubes inside the testes
–where spermatogenesis occurs (p.477)
3. epididymis
- coiled tubes leading from the testes where sperm are stored to mature and become motile
4. vas deferens
(sperm duct) - tube leading from the epididymis which extends upward into the abdominal cavity and through which sperm travel
–here sperm are mixed with fluid from a series of glands which include....
7.seminal vesicles
- produce mucous-like fluid containing fructose (sugar) to give sperm energy to move
9. Prostate gland-
secrete milky alkaline fluid to neutralize the acids in the female reproductive system (so sperm aren’t immediately destroyed)
5. Cowper’s (bulbourethral) gland
- two small glands on each side of the urethra that secrete a clear alkaline, lubricating fluid.
semen (not shown)
- combination of sperm and fluids
10. urethra
- passageway through which both urine and sperm exits the body
11. penis
- male reproductive organ which transfers sperm into female reproductive system
Other labels on diagram that aren't part of the 'male reproductive system"
6. rectum (passageway for feces)
8. urinary bladder (storage area for urine)
2. testes
- outside the body cavity
–produce male gamete (sperm) and reproductive hormones
–develop in the body cavity but descend into the ...
1. scrotum
- external sac which surrounds the testes
–allows the testes to remain ~ 1.5 degrees celcius below body temp for normal sperm production
•seminiferous tubules
- long coiled tubes inside the testes
–where spermatogenesis occurs (p.477)
3. epididymis
- coiled tubes leading from the testes where sperm are stored to mature and become motile
4. vas deferens
(sperm duct) - tube leading from the epididymis which extends upward into the abdominal cavity and through which sperm travel
–here sperm are mixed with fluid from a series of glands which include....
7.seminal vesicles
- produce mucous-like fluid containing fructose (sugar) to give sperm energy to move
9. Prostate gland-
secrete milky alkaline fluid to neutralize the acids in the female reproductive system (so sperm aren’t immediately destroyed)
5. Cowper’s (bulbourethral) gland
- two small glands on each side of the urethra that secrete a clear alkaline, lubricating fluid.
semen (not shown)
- combination of sperm and fluids
10. urethra
- passageway through which both urine and sperm exits the body
11. penis
- male reproductive organ which transfers sperm into female reproductive system
Other labels on diagram that aren't part of the 'male reproductive system"
6. rectum (passageway for feces)
8. urinary bladder (storage area for urine)
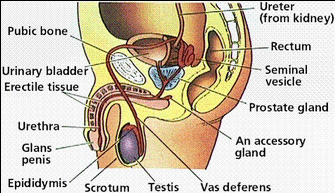
Labelled diagram of the male reproductive system (the accessory gland is the Cowper's).
Objective 4 & 5 - notes given in class
Male Sex Hormones: FSH, Inhibin, LH & Testosterone
FSH & Inhibin work in negative feedback loop
•FSH (follicle stimulating hormone)
–produced by anterior pituitary
–Stimulate seminiferous tubules in testes to produce sperm
•Inhibin
–produced by seminiferous tubules
–Targets hypothalamus to decrease the release of FSH from ant. pit.
Together they control the rate of sperm production.
LH & Testosterone also work in a negative feedback loop
•LH (luteinizing hormone)
–Producedby anterior pituitary
–Stimulates interstitial cells of testes to increase the production of testosterone
•Testosterone
–Responsible for secondary sex characteristics
–An increase in testosterone causes LH suppression
Male Sex Hormones: FSH, Inhibin, LH & Testosterone
FSH & Inhibin work in negative feedback loop
•FSH (follicle stimulating hormone)
–produced by anterior pituitary
–Stimulate seminiferous tubules in testes to produce sperm
•Inhibin
–produced by seminiferous tubules
–Targets hypothalamus to decrease the release of FSH from ant. pit.
Together they control the rate of sperm production.
LH & Testosterone also work in a negative feedback loop
•LH (luteinizing hormone)
–Producedby anterior pituitary
–Stimulates interstitial cells of testes to increase the production of testosterone
•Testosterone
–Responsible for secondary sex characteristics
–An increase in testosterone causes LH suppression
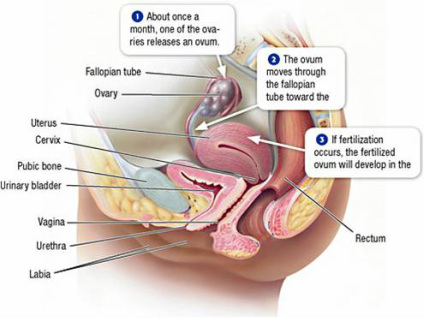
Objective 6 - originally given for homework
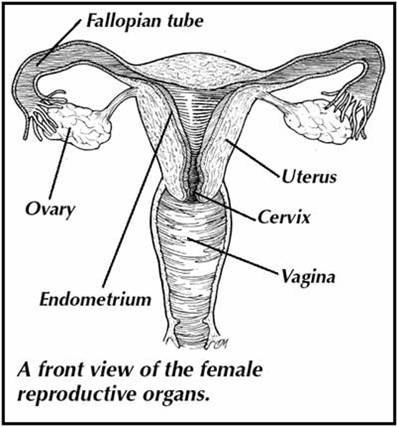
Structures of the female reproductive system p. 490-93
•ovary - suspended in the abdominal cavity
–produce female gamete (ovum or egg) and reproductive hormones
•follicles
- groups of cells in the ovaries
–each cell contains an ovum that may develop
oviduct (fallopian tube)
- pair of tubes that transport an ovum from
the ovary to the uterus
•fimbriae
- finger-like projections that sweep the egg from the ovary into the fallopian tube to direct it to the uterus
•uterus
- muscular organ in which the embryo develops
•endometrium
- the lining of the uterus which is richly supplied with blood vessels to supply nutrients to a developing fetus
•cervix
- muscular ring of tissue that separates the uterus and the vagina
• vagina
- canal that leads to the uterus
–allows entry of sperm into the females body
–functions as the birth canal
Structures of the female reproductive system p. 490-93
•ovary - suspended in the abdominal cavity
–produce female gamete (ovum or egg) and reproductive hormones
•follicles
- groups of cells in the ovaries
–each cell contains an ovum that may develop
oviduct (fallopian tube)
- pair of tubes that transport an ovum from
the ovary to the uterus
•fimbriae
- finger-like projections that sweep the egg from the ovary into the fallopian tube to direct it to the uterus
•uterus
- muscular organ in which the embryo develops
•endometrium
- the lining of the uterus which is richly supplied with blood vessels to supply nutrients to a developing fetus
•cervix
- muscular ring of tissue that separates the uterus and the vagina
• vagina
- canal that leads to the uterus
–allows entry of sperm into the females body
–functions as the birth canal
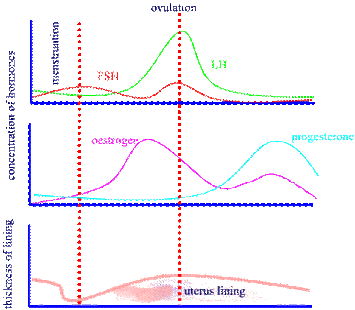
Female Hormones - Objective 7 - class notes
FSH (Follicle stimulating hormone) – released by anterior pituitary.
Several follicles begin to mature, but only one reaches maturity. Follicles releases estrogen.
estrogen - thickening of endometrium (lining of the uterus), inhibits FSH (negative feedback loop); causes increase in LH
LH (leutinizing hormone)- triggers release of ovum (ovulation); follicle producing ovum becomes corpus luteum; releases progesterone
progesterone - inhibits development of other follicles (low FSH); inhibits LH; as LH levels decrease, corpus luteum breaks down, and progesterone levels therefore decrease... leading to menstruation.
Objective 8 - path of sperm and egg until they meet (fertilization)
Egg (a.k.a. ovum) in follicle of ovary is released --> swept by fimbriae into oviduct (a.k.a. fallopian tube).If fertilization is going to occur as per normal, it would occur here.
Sperm is released by epididymis of testes into vas deferens (sperm duct) where fluid from the seminal vesicles, prostate, and cowper's gland is added. Sperm moves into urethra and out of penis into the vaginal canal. Sperm passes through cervix, into and through the urethra, and then to the oviduct, where it meets the egg and fertilization occurs.
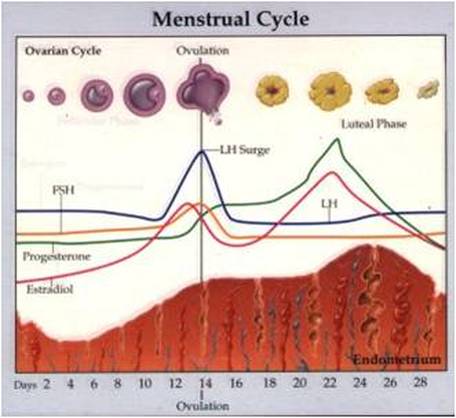
The Menstrual Cycle - Objective 9 & 10 - class handout
Follicular Stage (10-14 days)
•An increase of FSH stimulates the follicles
•The follicles cause a release of estrogen
•Estrogen causes the development of uterine lining, but also a decrease in FSH (negative
feedback loop)
Ovulation – ~ day 14
•As estrogen increases, so does LH
•Once LH reaches a certain level, the follicle breaks, causing the release of an ovum
(mature egg) - ovulation
Luteal Stage (Corpus Luteum Stage) – lasts 10-14 days
•Once the ovum is released, LH causes the follicle fills with cells forming the corpus luteum
•The corpus luteum releases progesterone (and some estrogen)
•Progesterone does several things
–prevents any other follicles from maturing (inhibits FSH)
–continues the growth of the uterine lining
–causes a decrease in LH (negative feedback loop)
Menstruation (3-5 days)
•As LH decreases, it causes the corpus luteum
to break down –causing a decrease in progesterone & estrogen
•As progesterone levels decrease, so does the blood supply to the endometrium
•The endometrium starts to break down and passes out through the vagina.
•As Estrogen drops, pituitary starts to increase the release of FSH and new follicles start to mature.
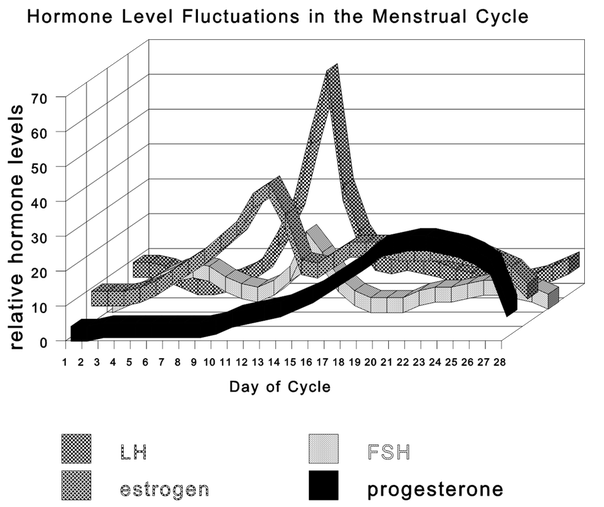
**It is important to note that most diagrams/graphs start and finish with the menstruation part of the cycle. It is usually considered the 'first stage' in the menstrual cycle (so the end of a graph is often the beginning of a 'new' cycle).
FSH (Follicle stimulating hormone) – released by anterior pituitary.
Several follicles begin to mature, but only one reaches maturity. Follicles releases estrogen.
estrogen - thickening of endometrium (lining of the uterus), inhibits FSH (negative feedback loop); causes increase in LH
LH (leutinizing hormone)- triggers release of ovum (ovulation); follicle producing ovum becomes corpus luteum; releases progesterone
progesterone - inhibits development of other follicles (low FSH); inhibits LH; as LH levels decrease, corpus luteum breaks down, and progesterone levels therefore decrease... leading to menstruation.
Objective 8 - path of sperm and egg until they meet (fertilization)
Egg (a.k.a. ovum) in follicle of ovary is released --> swept by fimbriae into oviduct (a.k.a. fallopian tube).If fertilization is going to occur as per normal, it would occur here.
Sperm is released by epididymis of testes into vas deferens (sperm duct) where fluid from the seminal vesicles, prostate, and cowper's gland is added. Sperm moves into urethra and out of penis into the vaginal canal. Sperm passes through cervix, into and through the urethra, and then to the oviduct, where it meets the egg and fertilization occurs.
The Menstrual Cycle - Objective 9 & 10 - class handout
Follicular Stage (10-14 days)
•An increase of FSH stimulates the follicles
•The follicles cause a release of estrogen
•Estrogen causes the development of uterine lining, but also a decrease in FSH (negative
feedback loop)
Ovulation – ~ day 14
•As estrogen increases, so does LH
•Once LH reaches a certain level, the follicle breaks, causing the release of an ovum
(mature egg) - ovulation
Luteal Stage (Corpus Luteum Stage) – lasts 10-14 days
•Once the ovum is released, LH causes the follicle fills with cells forming the corpus luteum
•The corpus luteum releases progesterone (and some estrogen)
•Progesterone does several things
–prevents any other follicles from maturing (inhibits FSH)
–continues the growth of the uterine lining
–causes a decrease in LH (negative feedback loop)
Menstruation (3-5 days)
•As LH decreases, it causes the corpus luteum
to break down –causing a decrease in progesterone & estrogen
•As progesterone levels decrease, so does the blood supply to the endometrium
•The endometrium starts to break down and passes out through the vagina.
•As Estrogen drops, pituitary starts to increase the release of FSH and new follicles start to mature.
**It is important to note that most diagrams/graphs start and finish with the menstruation part of the cycle. It is usually considered the 'first stage' in the menstrual cycle (so the end of a graph is often the beginning of a 'new' cycle).
Objective 11
Female Hormone Treatments
menopause - period in a woman's life where a decrease in estrogen and progesterone results in an end of menstrual cycles.
- due to a reduction in functioning follicles
- cessation of menstruation
During Menopause
- cholesterol levels rise
- bone mass declines
- blood vessels alternately constrict and dilate (hot flashes)
- mood changes
hormone replacement therapy- administration of low levels of estrogen and/or progesterone to
alleviate symptoms of menopause.
- debate ensuing
benefits of replacement therapy
- relief of symptoms of hot flashes
- prevention of bone loss
- improved memory
- dereased risk of UTI's
- decreased rate of macular degeneration (leading cause of blindness)
Risks of using estrogen in hormone replacement
- irregular vaginal bleeding
- stomach upset
- severe headache
- blood clots
- increased risk of breast cancer
Risks of using progesterone
- irregular vaginal bleeding
- stomach upset
- edema (water retention)
Risks of using both
- blood clots
- headache
- edema
- symptoms similar to PMS
- fluctuations in blood sugar
- increased risk of heart attack the first year
Female Hormone Treatments
menopause - period in a woman's life where a decrease in estrogen and progesterone results in an end of menstrual cycles.
- due to a reduction in functioning follicles
- cessation of menstruation
During Menopause
- cholesterol levels rise
- bone mass declines
- blood vessels alternately constrict and dilate (hot flashes)
- mood changes
hormone replacement therapy- administration of low levels of estrogen and/or progesterone to
alleviate symptoms of menopause.
- debate ensuing
benefits of replacement therapy
- relief of symptoms of hot flashes
- prevention of bone loss
- improved memory
- dereased risk of UTI's
- decreased rate of macular degeneration (leading cause of blindness)
Risks of using estrogen in hormone replacement
- irregular vaginal bleeding
- stomach upset
- severe headache
- blood clots
- increased risk of breast cancer
Risks of using progesterone
- irregular vaginal bleeding
- stomach upset
- edema (water retention)
Risks of using both
- blood clots
- headache
- edema
- symptoms similar to PMS
- fluctuations in blood sugar
- increased risk of heart attack the first year
| sti_table.docx | |
| File Size: | 15 kb |
| File Type: | docx |
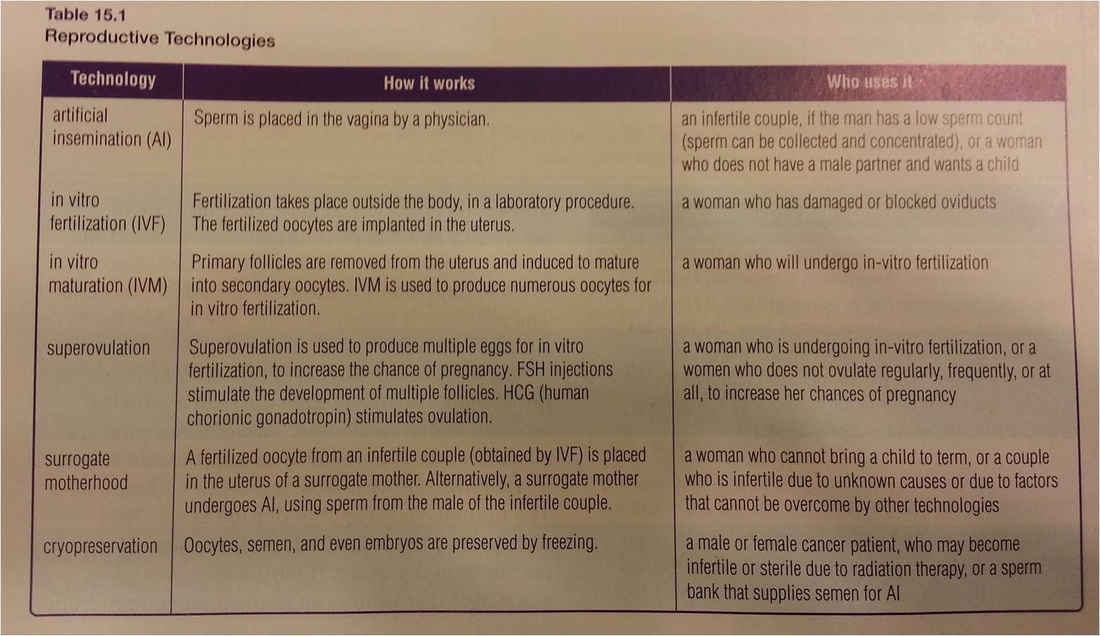
Conditions causing Infertility in females - Objective 13 p. 500-01
•Blocked oviducts – caused by PID (pelvic inflammatory disease), often caused by STI’s
•Failure to ovulate – caused by hormonal imbalances that occur for a variety of reasons, including being over or under weight.
•Endometriosis – painful condition in which the endometrium grows outside of the uterus.
•Damaged eggs – due to environmental factors, such as exposure to chemicals
Conditions causing Infertility in Males - Objective 13 p. 500-01
•Obstruction - in the vas deferens or epididymus, which may be caused by complications due to STI’s or varicose veins in the testes
•Low sperm count –caused by things like overheated testicles, smoking and alcohol consumption
•High proportion of abnormal sperm - caused by overheated testicles, exposure to toxins, or STI infections.
•Blocked oviducts – caused by PID (pelvic inflammatory disease), often caused by STI’s
•Failure to ovulate – caused by hormonal imbalances that occur for a variety of reasons, including being over or under weight.
•Endometriosis – painful condition in which the endometrium grows outside of the uterus.
•Damaged eggs – due to environmental factors, such as exposure to chemicals
Conditions causing Infertility in Males - Objective 13 p. 500-01
•Obstruction - in the vas deferens or epididymus, which may be caused by complications due to STI’s or varicose veins in the testes
•Low sperm count –caused by things like overheated testicles, smoking and alcohol consumption
•High proportion of abnormal sperm - caused by overheated testicles, exposure to toxins, or STI infections.

15. Controlling Reproduction – Contraception p. 502
•Surgery (vasectomy, tubal ligation)
•Hormonal (pill, needle, implant, morning-after pill)
•Physical barrier (diaphragm, cervical cap, condom, female condom)
•Avoidance (abstinence, rhythm method)
•Other (IUD, spermicide)
http://www.docstoc.com/docs/536159/Birth-Control-Chart
•Surgery (vasectomy, tubal ligation)
•Hormonal (pill, needle, implant, morning-after pill)
•Physical barrier (diaphragm, cervical cap, condom, female condom)
•Avoidance (abstinence, rhythm method)
•Other (IUD, spermicide)
http://www.docstoc.com/docs/536159/Birth-Control-Chart